
A colonoscopy is not supposed to be a financial personality test.
It is a routine prevention tool. A camera, a short procedure, a day off, a few awkward jokes, and a result that ideally buys you ten years of peace. That is the normal story.
In the United States, it is often not the normal story. It can become a bill maze with multiple actors, multiple codes, and multiple opportunities for the system to decide that “preventive” magically became “diagnostic” the moment anything slightly real happened. In France, it is usually boring in the way medical prevention should be boring. The costs are structured, the patient share is structured, and the whole thing is treated less like a retail transaction.
That is how you end up with the same basic screening experience producing numbers that feel like they belong to different planets.
A typical French patient pathway can leave you with something like €60 to €90 out of pocket in a standard situation, which is why people talk about an €80 bill as a normal, non-dramatic example. In the U.S., uninsured or cash-pay pricing can commonly run $1,300 to $4,200 depending on location and facility, and that range often does not include every add-on in every case. That is how someone ends up staring at $4,200 for what is supposed to be routine prevention.
This article is not about “France good, America bad” as a mood. It is about mechanisms. Why does the U.S. make prevention expensive and confusing while France makes it comparatively predictable, even when nothing is truly free?
The Procedure Is Similar The Billing Architecture Is Not
A colonoscopy is a colonoscopy in both countries.
There are variations in sedation practice, where it’s performed, and how follow-up is scheduled. But the core service is not exotic. It is an endoscopic exam of the colon, sometimes with biopsy or polyp removal.
The difference is the architecture around it.
In France, there is a national tariff logic. The act is coded. The base price is known. The reimbursement share is known. The remaining patient share is known. Then complementary coverage often mops up most of what’s left. You can still get extra charges, especially with certain doctors or certain private settings, but the starting point is regulated predictability.
In the U.S., the bill is often a pile of bills: facility fee, physician fee, anesthesia fee, pathology, pre-op consults, and sometimes surprise out-of-network elements that appear even when you tried to do the right thing. The result is that Americans often do not know what the price will be until after it happens, and sometimes not even then.
That is why Americans keep getting stuck. They are not only paying more. They are paying blind.
Why €80 Happens In France

Let’s be specific, because “France is cheaper” is not useful on its own.
France uses a coding and tariff framework for medical acts. For a standard colonoscopy act (a total colonoscopy code in the CCAM family), you’ll see a regulated base tariff around €153.60. Sedation or anesthesia is commonly billed separately, with a regulated base around €49.85 to €50.58 depending on the exact code context.
Add those together and you’re in the neighborhood of about €200 on regulated bases before any extras.
Then comes the reimbursement logic. For many acts, the statutory health insurance covers a percentage of the base tariff, and the remaining “ticket modérateur” is the patient share. For a colonoscopy example breakdown, one consumer-facing explainer that uses the standard convention tariff shows a remainder around €61 for the colonoscopy act plus anesthesia on the regulated bases, before complementary coverage.
France also has specific fixed patient contributions for certain acts. One of the big ones is the €24 fixed charge that can apply to costly acts above a threshold, replacing the normal percentage ticket modérateur in those cases.
So how do people land around €80?
In real life, the out-of-pocket total often looks like a stack of small, predictable items:
- a regulated remainder on the act and anesthesia
- possible fixed contributions like the €24 charge where applicable
- small participation charges on consultations
- possibly a small daily hospital charge if there’s an overnight stay, depending on setting and coverage
Then, for many residents, a mutuelle (complementary insurance) covers most or all of these, especially the ticket modérateur. That is why plenty of people end up near zero, while others land in a modest two-digit range.
The point is not that “France always costs €80.” The point is that France makes an €80 outcome plausible and normal for a routine pathway because the pricing is structured and the remaining patient share is bounded by design.
Why $4,200 Happens In America
Now let’s look at the U.S. side without pretending every colonoscopy is $4,200.
Many people pay less. Some people pay nothing for a truly preventive screening colonoscopy under their insurance rules. But plenty of people still get hit with large bills because the American system is full of conversion traps.
For uninsured or cash-pay patients, the range itself tells you what kind of country this is. A state-level pricing reference for New York lists typical cash prices from $1,300 to $4,200. Another consumer pricing guide shows a national average around $2,412 with a range up to $4,616 depending on setting and factors.
So yes, $4,200 is not a fantasy number.
And the reason it shows up is not because the procedure is four thousand dollars more complicated in America. It is because the American system prices procedures through a layered marketplace:
- hospital outpatient departments can price higher than ambulatory surgical centers
- anesthesia billing can be separate and expensive
- pathology can add cost when biopsies or polyps happen
- negotiated rates vary widely between insurers and facilities
- uninsured pricing can be punitive and inconsistent
The U.S. also has a particularly nasty feature for preventive care: if the screening becomes “diagnostic” in billing terms, patients can be exposed to deductibles and coinsurance even though the whole point was prevention.
That is how a routine screening turns into a financial event.
The Hidden Cost Is Fear, Not Just Money
Even when the dollar amount is not catastrophic, the U.S. system teaches fear.
It teaches people to delay. To shop procedures like flights. To avoid follow-up. To treat prevention as optional because “what if it costs something insane.” It teaches people to tolerate symptoms longer because every step triggers a billing risk.
France has its own frustrations, but it does not generally teach the same kind of fear about basic care. A French resident might complain about wait times, paperwork, or finding the right specialist. The complaint is rarely “I’m afraid a screening will destroy my finances.”
That emotional difference has consequences.
Heart disease, colon cancer, diabetes, and many other conditions get worse when prevention is delayed. So even if you ignore morality and focus only on outcomes, a system that makes prevention financially predictable will usually catch more problems earlier.
A system that prices prevention like a luxury product will catch fewer problems early, and then spend more on late-stage damage.
That is the part Americans often miss. Expensive prevention is not “saving money.” It is buying worse outcomes later.
Why France Can Keep Prices Predictable
France’s predictability is not a cultural miracle. It is policy design.
The country operates a social health insurance model with regulated tariffs for many services. Reimbursement is calculated based on set reference rates. Complementary insurance commonly covers cost-sharing, which is why out-of-pocket at the point of care can be low for many people, even when the underlying service has a real cost.
A key detail: France’s system is built to make the patient legible and the price legible. The act has a known tariff base. The reimbursement share is known. The remaining share is knowable.
That predictability is not just nice. It is a public health tool.
You cannot build mass screening programs if each screening is a financial surprise.
Why America Keeps Producing Surprise Bills
The U.S. has a different design goal. It does not behave like a national health system. It behaves like a health care market with insurance as the gatekeeper.
That creates two problems for prevention:
- price fragmentation
- classification games
Price fragmentation is the obvious part: multiple entities, multiple bills, multiple negotiated rates, and massive variation by location and facility type.
Classification games are the sneaky part: preventive versus diagnostic, in-network versus out-of-network, facility versus physician, billed under one code versus another.
Even people who have insurance can get hit with large charges if the colonoscopy is coded in a way that triggers cost-sharing. Even people who tried to pick the right facility can get a surprise component from anesthesia or pathology. Even people who thought they were covered can learn after the fact that “covered” is not the same as “paid for.”
This is why Americans talk about “billing surprises” as if that is just how adult life works.
It is not.
It is how a poorly designed financing model works.
The Middle-Aged Reality Check
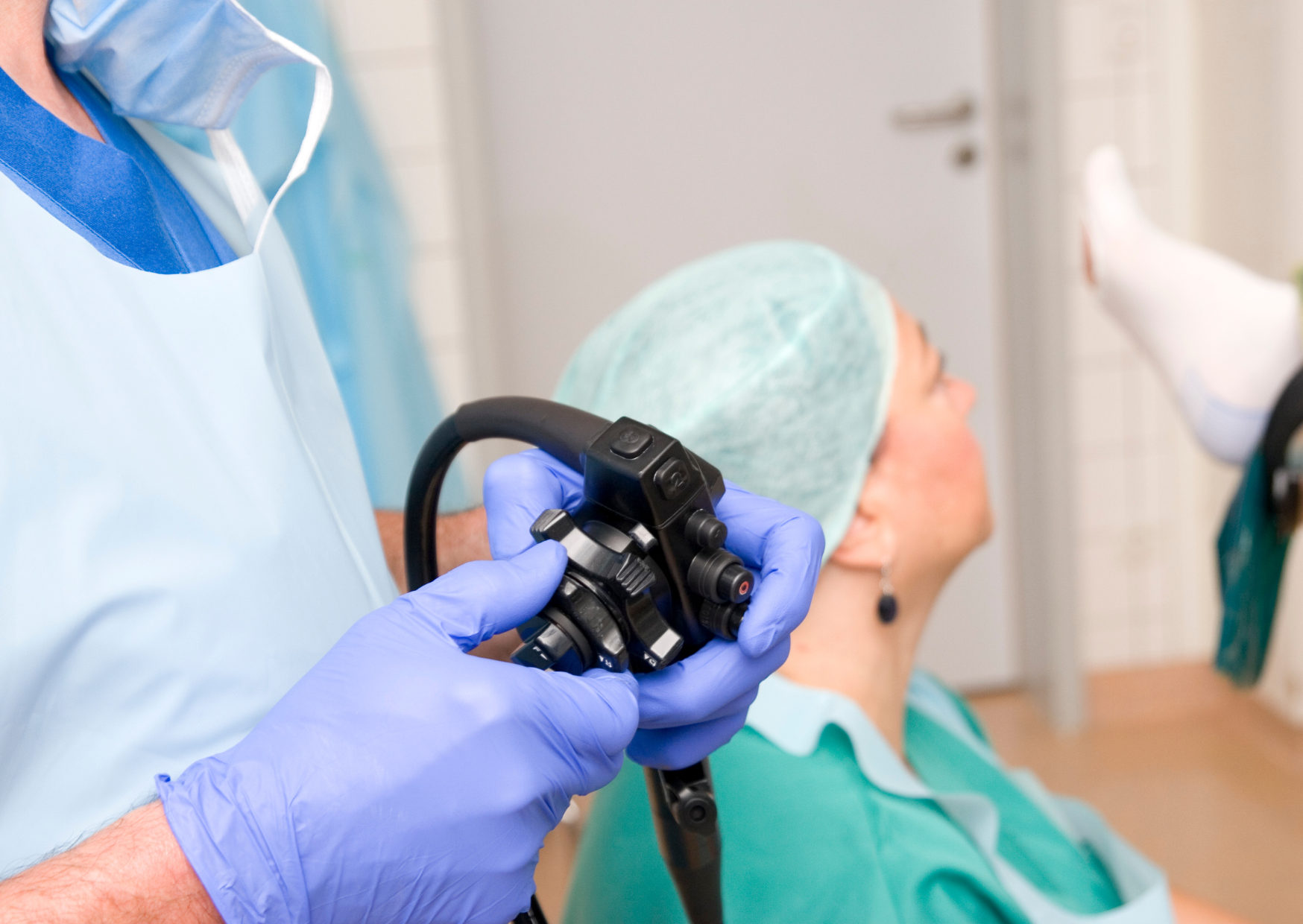
If you are 45 to 65, this topic is not academic.
This is the window where prevention starts paying off or starts getting postponed. This is also the window where people often have higher deductibles, more complicated insurance, and more financial pressure. The U.S. system is very good at making a 55-year-old feel like they should “wait until next year” for basic screenings.
That habit has real consequences.
Colon cancer is one of the clearest examples because screening can directly prevent cancer by removing polyps. The whole point is to do it before anything feels urgent.
France’s pricing structure supports that logic.
America’s pricing structure often fights it.
This is one of the reasons Americans abroad feel shocked. They are not shocked because France is free. They are shocked because prevention is treated like normal infrastructure rather than a consumer purchase.
The First 7 Days To Get A Real Price Before You Commit

If you are in the U.S. and you want to avoid becoming the person with the $4,200 bill, you need to treat this like a negotiation with a system that does not behave honestly by default.
Here’s the seven-day plan that actually works.
Day 1
Find out whether your colonoscopy is being scheduled as screening or diagnostic. Do not accept vague language. That classification is the difference between “covered” and “you owe a lot.”
Day 2
Ask for the CPT and diagnosis codes that will be used. You are not being difficult. You are being realistic.
Day 3
Call your insurer and ask what you will owe under those codes at that facility. Ask specifically about anesthesia and pathology. If they cannot answer, ask how to get a written estimate.
Day 4
Ask the facility for an all-in estimate including physician, facility, anesthesia, and pathology. If they say they cannot, ask for typical ranges and whether anesthesia is in-network.
Day 5
If you are cash-pay, ask for the cash price and whether it includes anesthesia and pathology. Cash prices exist. They vary. They can sometimes be negotiated.
Day 6
If you have access to an ambulatory surgical center, compare it with a hospital outpatient setting. Site-of-service pricing differences can be enormous.
Day 7
Decide with your eyes open. If your out-of-pocket is high, ask about alternatives like fecal immunochemical tests as an interim tool, but do not let “too expensive” become a permanent avoidance habit.
This is not how prevention should work. It is how you survive the U.S. system as it exists.
The Honest Takeaway
A colonoscopy is not supposed to be a luxury product.
France does not make it free. France makes it predictable.
The U.S. does not always make it impossible. The U.S. makes it unstable, and instability is enough to delay people.
That delay is deadly in slow, boring ways.
When a country can’t make routine prevention routine, it ends up spending more money later while still losing people earlier. That is the worst possible deal: expensive and worse.
So yes, the same basic preventive tool can land around €80 in France for a typical, regulated pathway, while landing around $4,200 in the U.S. for a cash-pay patient in many settings.
The shocking part is not the number.
The shocking part is what the number reveals: one country treats prevention as infrastructure, and the other treats it as a market transaction with traps.
About the Author: Ruben, co-founder of Gamintraveler.com since 2014, is a seasoned traveler from Spain who has explored over 100 countries since 2009. Known for his extensive travel adventures across South America, Europe, the US, Australia, New Zealand, Asia, and Africa, Ruben combines his passion for adventurous yet sustainable living with his love for cycling, highlighted by his remarkable 5-month bicycle journey from Spain to Norway. He currently resides in Spain, where he continues sharing his travel experiences with his partner, Rachel, and their son, Han.
