The first time you try to refill an American prescription in Europe, you learn a harsh truth fast: your prescription is not a passport.
In the US, a prescription feels like a clean, portable thing. A doctor wrote it. A pharmacy fills it. You pay. You leave. If you move states, it’s annoying, but it’s still basically the same system.
Europe doesn’t work that way. Not because Europeans are anti-medicine or because they enjoy watching foreigners suffer. It’s because prescriptions are tied to local licensing, local rules, local formularies, local insurance systems, and local responsibility.
So what happens is predictable:
- You arrive with a US medication routine that has worked for years.
- You assume you can “just transfer it.”
- A pharmacist looks at your paper, shrugs, and says some version of no.
- You panic because this medication is not optional.
- Then you start hearing the phrase that drives Americans insane: “You need to see a doctor here.”
This article is the reality-based guide: what usually works, what doesn’t, and the practical workarounds people actually use in Spain and across Europe when they need continuity without doing something reckless.
Why US prescriptions don’t automatically work here

Start with the blunt mechanics.
A US prescription is issued under US licensing and US rules. European pharmacies and clinicians operate under their own national regulations and liability frameworks. A pharmacist in Spain can’t just take an American prescription for a controlled medication and decide to honor it because it seems legit. They’re accountable under Spanish law, and their dispensing authority is tied to Spanish and EU frameworks.
Also, Europe doesn’t run one unified prescription system. Even within the EU, healthcare is national. Formularies vary. Brand names vary. Pack sizes vary. Dosing conventions can vary. Coverage rules vary. Controlled substance rules vary.
So “I take Adderall 20 mg” or “I take Xanax” or “I take this specific brand of thyroid medication” lands differently depending on where you are.
That’s why the first rule is simple:
Assume you will need a local prescriber for ongoing meds.
Not eventually. Early.
Workarounds exist. But the long-term solution is almost always local continuity of care.
The medication types that cause the most trouble

Not all prescriptions are equal. Americans tend to assume the difficulty level is the same across the board. It isn’t.
1) Controlled substances
This is where most people hit a wall.
Common examples:
- stimulant ADHD medications
- benzodiazepines
- opioid pain medications
- some sleep meds
- some anxiety meds
Even if the medication exists in Europe, the prescribing culture may be stricter, the criteria may differ, and the refill rules may be tighter. Also, controlled drugs are where pharmacies and doctors are least interested in “trusting your story.”
They want documentation. They want diagnosis history. They want local oversight.
If your US prescription is a controlled substance, plan for friction. Don’t wing it.
2) Specialty meds and biologics
These can be available, but they often require specialist care and specific protocols. You may not be able to walk into a clinic and walk out with a refill. You may need referrals, hospital pharmacies, and structured monitoring.
3) Psychiatric meds
Non-controlled psych meds are often easier than controlled substances, but the system still expects local medical supervision.
Also, some drugs are used differently in Europe. A US regimen may not be standard. Doctors may want to adjust.
4) Hormone-related meds
This can be easy or hard depending on the medication and the diagnosis documentation you can provide. Some areas are routine. Others can be culturally and medically conservative.
5) Plain-vanilla chronic meds
Blood pressure meds, cholesterol meds, many diabetes meds, thyroid meds, asthma inhalers, common antibiotics. These are often the easiest category, though you still usually need local prescriptions.
Workarounds are easier when the drug is common, non-controlled, and not a specialist-only pathway.
The real strategy: stop chasing the exact brand, chase the active ingredient
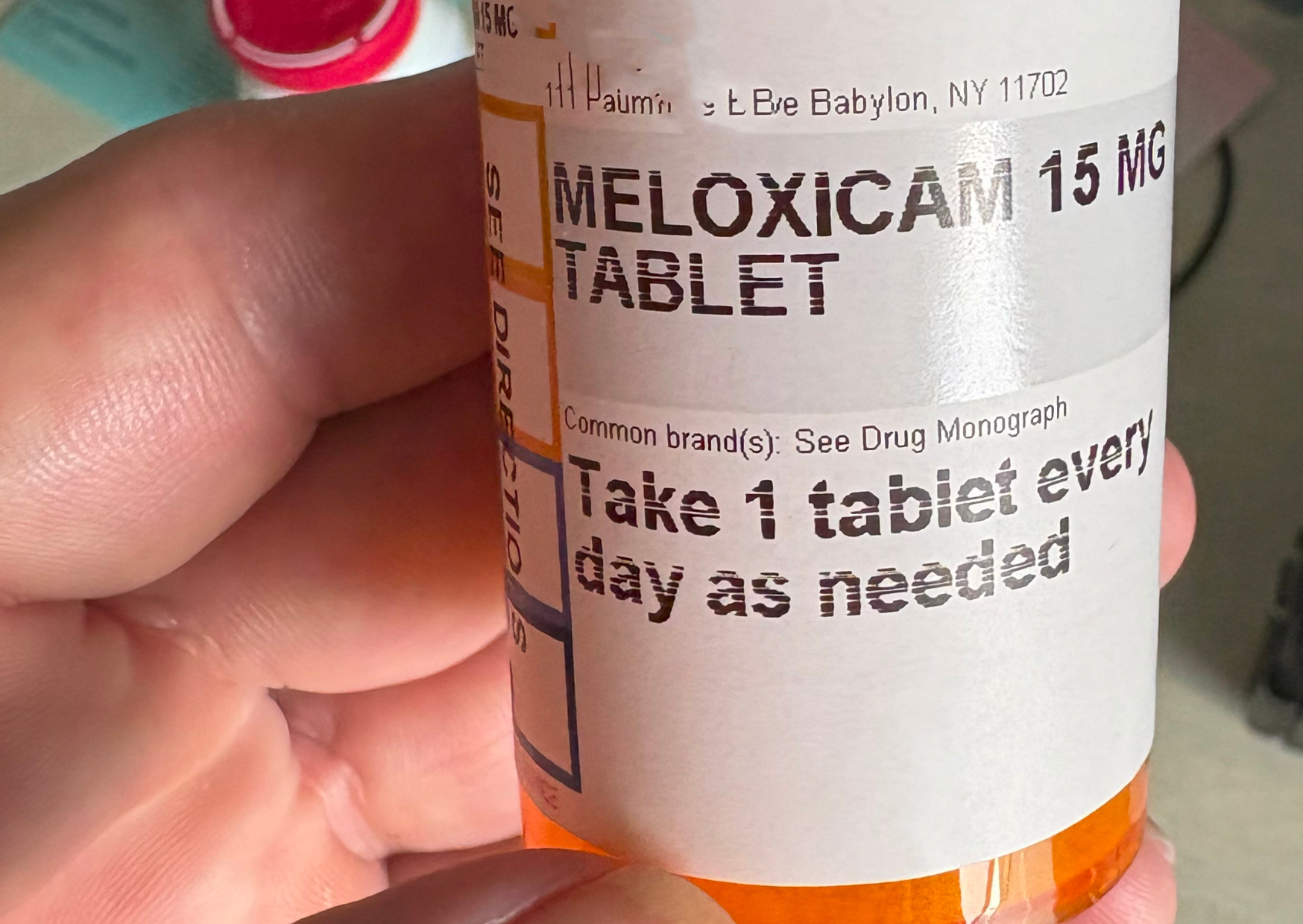
Americans get stuck on brand names. Europe tends to operate more around active ingredients and equivalents.
If you arrive insisting you need “Brand X,” you may waste weeks. If you arrive knowing:
- active ingredient name
- dosage
- formulation (immediate release vs extended release)
- how long you’ve been on it
- what you’ve tried and failed
You become much easier to help.
This is one of the biggest psychological shifts: treat your medication as a molecule, not a product.
Know your generic names. Know them cold.
Because even when your exact American brand exists, it may be marketed under a different name or packaged differently.
The documents that actually help you get continuity
If you want a European doctor to take over prescribing, you need to show them you’re not making it up. The more structured and boring your documentation is, the smoother it goes.
What helps most:
- A current medication list with dosages and timing
- A letter or summary from your US doctor stating diagnosis and treatment history
- Recent relevant labs (if applicable)
- A history of prior medications tried
- Any specialist notes (psychiatry, cardiology, endocrinology)
- Proof of ongoing monitoring (especially for controlled or higher-risk meds)
And here’s the key detail Americans miss: recency matters. A note from five years ago feels meaningless to many clinicians. You want documentation from the last year if possible.
Also, if you can get your doctor to write the summary in plain language, not clinic jargon, it helps. European clinicians may not share the exact same shorthand. Clear language beats medical poetry.
Your goal is to make your case easy to understand in 60 seconds. That’s how you get help.
Workaround 1: Book a local doctor fast, even if you don’t feel ready
This is the boring answer. It is also the correct one for most people.
If you know you’ll need refills, don’t wait until you have two pills left. Book a local appointment early.
In Spain, you’ll usually be navigating one of two tracks:
- public system access (if and when you’re eligible and registered)
- private care (self-pay or private insurance)
Newcomers often try to postpone this because they don’t want another administrative project. But medication continuity is not optional. Treat it like rent. It needs a plan.
Here’s what works in real life:
- Book a private GP visit early to establish a local medical record.
- Bring your documentation pack.
- Explain calmly: what you take, why you take it, how long you’ve taken it, what happens if you stop.
- Ask for the local equivalent and a plan for future refills.
Even if you plan to eventually rely on the public system, private is often the fastest way to bridge the first year.
Fastest bridge is often private GP, then transition. It’s not ideological. It’s timing.
Workaround 2: Use a specialist when the medication is specialist-governed

Some meds are simply not a GP casual refill situation. You need the correct specialist lane.
Examples:
- certain psychiatric meds
- certain neurological meds
- certain endocrine meds
- biologics and specialty injections
If you show up to a GP asking for something that specialists typically manage, you may get stalled. Not because the GP is mean, but because they’re cautious.
So the workaround is: accept that your first step is often a GP referral or a private specialist appointment.
Yes, it’s annoying. But it’s usually faster than trying to convince a GP to do something outside their comfort lane.
Don’t argue the lane. Enter the correct lane.
Workaround 3: Bring a supply legally, but don’t build your life around suitcases
A lot of Americans do the “stock up and bring it” approach. Sometimes that’s necessary as a bridging tactic. But it has limits.
You need to think about:
- how much you are legally allowed to travel with
- whether the medication is controlled where you are going
- whether you need documentation to show at borders
- whether the supply is stable (some meds require refrigeration)
- the risk of loss, theft, or travel disruptions
Also, relying on US refill trips as your core strategy is fragile. It works until it doesn’t:
- you get sick and can’t travel
- flights get disrupted
- life gets busy
- your US doctor wants an in-person visit
- your insurance changes
- the medication gets harder to refill in the US
Use travel supply as a temporary buffer, not as a long-term system.
A buffer is smart. A suitcase strategy is brittle.
Workaround 4: Use EU pharmacy reality: ask for equivalents, not miracles
Pharmacists in Europe can be incredibly helpful, but you need to ask the right way.
If you walk in saying, “Can you fill this American prescription,” the answer is often no.
If you walk in saying:
- “I take this active ingredient, this dose, this formulation.”
- “What is the equivalent here?”
- “Is it prescription-only here?”
- “What doctor type usually prescribes it?”
You get useful information even when you can’t get the medication that day.
Pharmacists can often tell you:
- whether the drug exists locally
- what the local name is
- what the typical prescribing pathway is
- whether there’s a similar alternative
- what documentation a doctor might want
This turns the pharmacy from a dead end into an intel source.
Use pharmacists as navigators, not vending machines.
Workaround 5: Telemedicine can help, but it’s not magic
Telemedicine in Europe can be useful for basic issues and routine meds, especially if you are already in a system and need a minor refill.
But it’s not a guaranteed solution for:
- controlled substances
- complex psychiatric meds
- high-risk meds
- anything requiring monitoring or specialist involvement
Also, telemedicine providers may be conservative with foreigners they haven’t seen, especially if your documentation is thin.
The correct use of telemedicine is:
- bridging simple refills
- getting an initial GP consult when you can’t get an appointment quickly
- having a clinician direct you to the appropriate pathway
Don’t treat telemedicine as “US-style refill vending.” That expectation is where people waste money and time.
Telemedicine is a tool. It’s not a loophole.
Workaround 6: Private insurance helps with access, not with rules
Americans assume private insurance means “the rules disappear.” No. It means access can be faster and choice can be wider.
You still need:
- a local prescriber
- a legitimate diagnosis pathway
- documentation
- and compliance with controlled substance policies
Private insurance can shorten the queue. It doesn’t eliminate legal frameworks.
It also doesn’t guarantee you’ll get the exact medication you got in the US. A doctor can still say: we do it differently here.
So private insurance is best treated as:
- a speed tool
- an appointment tool
- a specialist access tool
Not as a medication guarantee.
Insurance buys access. It doesn’t buy entitlement.
Workaround 7: Accept substitutions and rebuild your regimen safely
This is the hard one emotionally. People don’t like change when it comes to meds. Fair.
But sometimes the only path is substitution. The medication you used in the US is not commonly prescribed where you are. Or it’s available but tightly controlled. Or the formulation is different.
So you may need to rebuild your regimen with a local clinician.
If you go into that conversation with a rigid “no changes” stance, you may stall. If you go in with a “here’s what works for me, here are my non-negotiable outcomes, let’s find a safe equivalent” stance, you’re more likely to get continuity.
Key point: substitutions should be medical decisions, not pharmacy experiments. Don’t DIY your regimen because someone in a Facebook group said “it’s basically the same.” Get clinician oversight.
Flexibility gets you care. Recklessness gets you instability.
The situations where you should not mess around
Some conditions and meds are not the place for internet workarounds. If your medication supports something high-stakes, treat it that way.
Examples:
- seizure control
- insulin-dependent diabetes management
- anticoagulants
- transplant meds
- severe psychiatric stability
- serious pain management
- anything where abrupt discontinuation is dangerous
In these cases, your strategy should be:
- get local medical oversight early
- build a bridging supply buffer legally
- bring your documentation pack
- and accept specialist lanes when required
If your medication is safety-critical, don’t let your pride about “not wanting to deal with doctors” create a medical crisis.
Your health is not the place to prove you’re independent.
The money reality: prescriptions can get cheaper, but access has costs
Some Americans arrive thinking medication will be dramatically cheaper in Europe. Sometimes it is, especially once you are integrated into a national system.
But newcomers often hit a different reality first:
- private appointment fees
- specialist fees
- time spent building access
- possible diagnostic re-evaluation
- upfront costs for visits and documentation
So yes, unit prices can be lower. But the first-year cost can still be significant because you’re paying for access and continuity building.
Also, if you are bridging through private care, costs can vary widely depending on:
- the city
- the clinic
- whether labs are needed
- whether specialist consults are required
The smartest approach is to treat the first six months as an integration phase with an upfront budget line.
Cheaper meds later doesn’t help if you can’t access them now.
The 7-day plan to stop gambling with your prescriptions
If you’re reading this because you’re low on meds, do this immediately. Not perfectly. Immediately.
Day 1: Build your medication dossier
One PDF pack:
- med list with generic names, doses, timing
- diagnosis summary
- recent doctor note
- relevant labs if applicable
- a photo of your current prescription bottles (labels matter)
Keep it in a folder you can send.
Day 2: Identify local equivalents
Go to a pharmacy and ask about the active ingredient equivalents and the prescribing pathway. Write down names and notes.
Day 3: Book a local appointment
Private GP is often fastest. Book it even if it’s not your ideal long-term solution.
Day 4: Prepare your ask
Write a short script:
- “I take X for Y. I’ve taken it since Z. I’m stable on it. I need continuity and local oversight.”
Keep it calm and factual.
Day 5: Build a buffer legally
If you can bring a legal supply through travel or existing refills, do it, but don’t let that replace the local appointment. It’s a buffer, not a system.
Day 6: If controlled or specialist, book the right lane
If your meds are controlled or specialist-driven, book the specialist consult now. Don’t wait for a GP to tell you what you already suspect.
Day 7: Decide your long-term track
- public system integration plan if eligible
- private plan if not
- documentation refresh routine every 6 to 12 months
This is how you stop living refill to refill like a stressed animal.
Documentation, appointment, buffer, then integration. That sequence saves people.
The honest takeaway: the workaround is a system, not a trick
Americans want the hack. The European reality is that continuity comes from building a local care pathway.
The workarounds that actually work are not glamorous:
- knowing your active ingredients
- having documentation ready
- using pharmacists for intel
- booking local doctors early
- accepting specialist lanes for certain meds
- using legal buffer supplies short-term
- being flexible about equivalents under clinician oversight
If you do those things, you can usually maintain stability. If you refuse them, you end up in panic mode, spending money, and making risky decisions.
The European system doesn’t care that you had a functioning life in the US. It cares that you now live here and need to be prescribed here.
Once you accept that, this stops being a nightmare and starts being a manageable integration task.
About the Author: Ruben, co-founder of Gamintraveler.com since 2014, is a seasoned traveler from Spain who has explored over 100 countries since 2009. Known for his extensive travel adventures across South America, Europe, the US, Australia, New Zealand, Asia, and Africa, Ruben combines his passion for adventurous yet sustainable living with his love for cycling, highlighted by his remarkable 5-month bicycle journey from Spain to Norway. He currently resides in Spain, where he continues sharing his travel experiences with his partner, Rachel, and their son, Han.
